Revolutionary Breakthrough: Protein Linked to Aging Joints Offers New Hope for Osteoarthritis Treatment
A groundbreaking study in mice has identified a single protein, 15-PGDH, as a key driver of cartilage loss associated with aging. This discovery opens new avenues for treating osteoarthritis, a debilitating condition affecting millions worldwide. Researchers believe targeting this protein could lead to therapies that restore mobility and significantly alleviate discomfort in older adults, marking a pivotal moment in regenerative medicine.
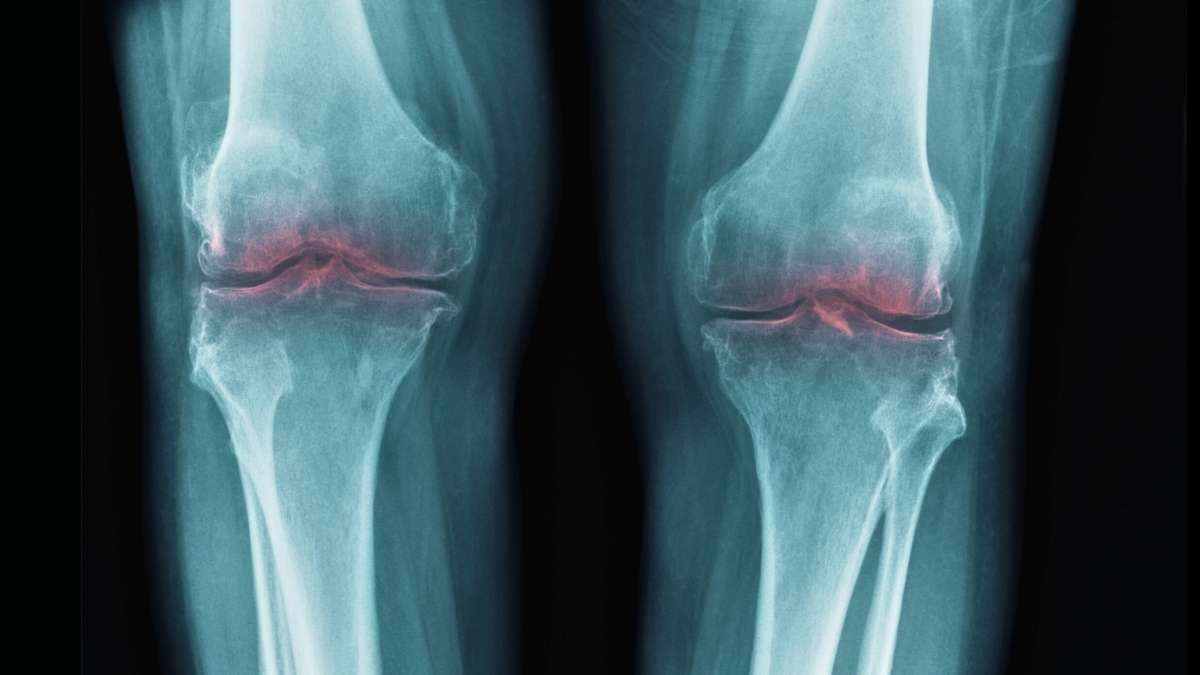
The relentless march of time often brings with it a host of physical challenges, none perhaps as pervasive and debilitating as the degradation of our joints. For millions globally, osteoarthritis (OA)—a chronic condition characterized by the breakdown of cartilage in joints—transforms everyday movements into agonizing ordeals. Until now, treatments have largely focused on managing symptoms rather than addressing the root cause. However, a recent, groundbreaking study conducted in mice has unveiled a startling revelation, pinpointing a single protein as a primary culprit in age-related cartilage loss, offering an unprecedented glimmer of hope for future therapeutic interventions.
This pivotal research, which has sent ripples through the scientific community, identified a protein known as 15-PGDH (15-hydroxyprostaglandin dehydrogenase). While 15-PGDH has long been recognized for its extensive links to the aging process, its direct role in the deterioration of articular cartilage remained largely unexplored. The findings suggest that by modulating the activity of this specific protein, scientists may be able to not only halt but potentially reverse the degenerative processes that lead to OA, promising a future where restored mobility and comfort are within reach for aging populations.
Unraveling the Mystery of Cartilage Degradation
Articular cartilage, the smooth, resilient tissue that covers the ends of bones in joints, acts as a natural shock absorber, enabling frictionless movement. Unlike many other tissues, cartilage has a limited capacity for self-repair, making its degradation particularly problematic. As we age, this vital tissue thins, frays, and eventually erodes, leading to the bone-on-bone friction characteristic of advanced osteoarthritis. The exact mechanisms driving this age-related decline have been a subject of intense scientific inquiry for decades.
The recent study focused on the intricate cellular processes within the joint, specifically examining how aging impacts chondrocytes—the specialized cells responsible for maintaining cartilage health. Researchers observed that as mice aged, there was a significant increase in the levels of 15-PGDH within their joint tissues. This elevation, they discovered, was directly correlated with a decrease in the production of prostaglandin E2 (PGE2), a crucial lipid mediator known for its protective and anabolic effects on cartilage. PGE2 plays a vital role in stimulating cartilage repair, reducing inflammation, and promoting the synthesis of essential cartilage components like collagen and proteoglycans.
Essentially, 15-PGDH acts as an enzyme that breaks down PGE2. Therefore, higher levels of 15-PGDH lead to lower levels of protective PGE2, creating an environment conducive to cartilage degradation. This mechanistic link provides a clear, actionable target for therapeutic development. "For years, we've been searching for the 'on/off switch' for cartilage health in aging," stated one of the lead researchers in a press release. "Identifying 15-PGDH as a key regulator of PGE2 in joints is a monumental step forward."
Historical Context and Current Treatment Landscape
Osteoarthritis is not a new disease; evidence of its presence has been found in ancient human remains. However, its prevalence has surged with increased life expectancy. Globally, OA affects hundreds of millions, making it a leading cause of disability. According to the World Health Organization, over 500 million people worldwide suffer from OA, with the knee and hip being the most commonly affected joints. The economic burden is staggering, encompassing healthcare costs, lost productivity, and the significant impact on quality of life.
Current treatment strategies for OA are largely palliative. They include: * Pain management: Over-the-counter pain relievers, NSAIDs, and prescription opioids. * Physical therapy: Strengthening muscles around the joint and improving flexibility. * Lifestyle modifications: Weight loss and low-impact exercise. * Injections: Corticosteroids or hyaluronic acid to reduce inflammation and lubricate the joint. * Surgery: Joint replacement (arthroplasty) for severe cases, which is invasive and carries risks.
While these approaches can offer temporary relief, none fundamentally address the progressive loss of cartilage. The advent of therapies targeting 15-PGDH could represent a paradigm shift, moving from symptom management to disease modification, potentially offering a true restorative solution.
The Promise of 15-PGDH Modulation
The most exciting implication of this research is the potential to develop drugs that specifically inhibit 15-PGDH. By reducing the activity of this protein, scientists hypothesize that they can increase the levels of PGE2 within the joint, thereby promoting cartilage regeneration and slowing or even reversing the degenerative process. Early experiments in mice have already shown promising results, with animals treated with a 15-PGDH inhibitor exhibiting significantly less cartilage damage and improved joint function compared to untreated controls.
This approach is particularly appealing because it targets an endogenous pathway—meaning it leverages the body's own mechanisms for repair and maintenance. Rather than introducing foreign substances or undergoing invasive procedures, the goal is to restore the natural balance within the joint. Furthermore, because 15-PGDH is already known to be involved in various aging processes, understanding its role in OA could unlock broader insights into age-related diseases.
However, the journey from mouse studies to human therapies is long and fraught with challenges. Researchers must rigorously test potential inhibitors for efficacy, safety, and long-term side effects. Clinical trials will be necessary to determine optimal dosages and patient populations. Yet, the scientific community is cautiously optimistic. "This isn't just another incremental step; it's a conceptual leap," remarked a leading rheumatologist not involved in the study. "If we can safely translate these findings to humans, it would be transformative for millions."
Looking Ahead: A Future of Regenerative Joint Health
The discovery of 15-PGDH's role in age-related cartilage loss marks a significant milestone in the quest to conquer osteoarthritis. It provides a tangible, molecular target for drug development, potentially paving the way for a new generation of therapies that could fundamentally alter the trajectory of the disease. Imagine a future where a simple intervention could prevent or even reverse the debilitating effects of OA, allowing individuals to maintain active, pain-free lives well into their senior years. This research not only offers hope for those currently suffering but also opens doors for proactive strategies to preserve joint health as populations continue to age globally.
While human trials are still some years away, the scientific foundation laid by this study is robust. The next phase will involve intensive drug discovery and preclinical testing, followed by the rigorous phases of clinical development. The promise of restoring mobility and easing discomfort for seniors, not through invasive surgery or temporary pain relief, but through targeted biological intervention, is a compelling vision that fuels the ongoing dedication of researchers worldwide. This breakthrough underscores the power of basic scientific inquiry to unlock profound solutions to some of humanity's most persistent health challenges.
Stay Informed
Get the world's most important stories delivered to your inbox.
No spam, unsubscribe anytime.
Comments
No comments yet. Be the first to share your thoughts!